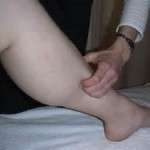
 Practice mistakes and bio-habitual irregularities are crucial risk conditions for aggravating shin splints, MTSS (medial tibial stress syndrome – shin splints). Your physician should do a comprehensive musculoskeletal checkup primarily concentrating on the lower-limbs. The mid-crease of the shinbone (medial ridge of the tibia) usually is sensitive to handle, primarily at the farthest and middle shin areas. The foremost shin (tibia) normally isn’t sensitive. Neurovascular problems are regularly non-existent.
Practice mistakes and bio-habitual irregularities are crucial risk conditions for aggravating shin splints, MTSS (medial tibial stress syndrome – shin splints). Your physician should do a comprehensive musculoskeletal checkup primarily concentrating on the lower-limbs. The mid-crease of the shinbone (medial ridge of the tibia) usually is sensitive to handle, primarily at the farthest and middle shin areas. The foremost shin (tibia) normally isn’t sensitive. Neurovascular problems are regularly non-existent.
Shin splints is related with bio-habitual defects of the lower-limbs, thus a doctor should finely diagnose for potential irregularities like femur anteversion, foot arch abnormalities, leg-length divergence, or a shin twist (tibial torsion). Ankle and tubular changes and subtalar movement should also be analyzed. Hyperpronation of the subtalar joint is a frequent risk condition for shin splints.
Muscle instability and rigidity particularly tightness of the triceps surae, is regularly an offshoot of shin splints. Athletic people with triceps muscle vulnerability are liable to languid muscles that provokes to enervated running faculties and hardship on the tibia. A doctor should also check for hamstring and quadriceps muscle rigidness and asymmetry.
Enervation of important muscles is a pressing risk condition for lower limb injuries. Hip and pelvis muscle fortitude is an acute component in cultivating stability and adequate mechanics between important muscles and the lower limbs. Important and pelvic muscle durability may be diagnosed by the patient’s capacity to manage a composed, balanced pelvis throughout a pelvic bridge from the supine location, or a standing single-leg knee bend.
Lower limb injuries are also associated with anatomical irregularities beyond the kinetic chain, detached from the injury site. A malfunctional spine, sacroiliac joint, and pelvis may perpetuate trauma of the lower limbs. So the doctor should do a standing postural examination to assess the whole kinetic chain, primarily if the symptoms are reoccurring. Musculoskeletal deficiencies (somatic dysfunctions) can be detected by a mnemonic TART (Tenderness, Asymmetry, Restricted motion, and Tissue texture) abnormality. These guidelines should be employed to the integral kinetic chain like the muscles, soft tissues and bones of the spine, pelvis, and lower-limbs. Several procedures are practiced to observe leg-length divergence. Probing the patient in a supine position, while assessing for a proportionate middle small-hammer (malleoli), is easy and effectual.
Evaluating a patient’s shoes may disclose dilapidated shoes or persistent impressions with leg-length divergence or disparate bio-habitual irregularities. An incongruous gait pattern should be judged with the patient walking or running, either on a treadmill or anywhere in the physician’s office with a lengthy walkway.





